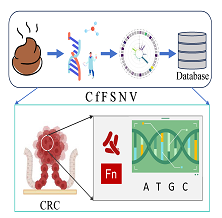
Fusobacterium nucleatum (Fn) is a Gram-negative anaerobic bacterium that has been most extensively studied in the development and progression of colorectal cancer (CRC). Although Fn is typically found in the oral cavity, it is also specifically enriched in the feces and tumor tissues of CRC patients. As a common oral colonizer, Fn can translocate to the gut when the oral-gut barrier is compromised. It promotes the occurrence and progression of CRC through various mechanisms, rewrites the tumor microenvironment, and facilitates metastasis and chemotherapy resistance. Current microbiome research in CRC primarily focuses on taxonomic composition and microbial functional capacities, often overlooking extensive microbial genomic variation. Such genomic variations, including structural variants, insertions and deletions, as well as single nucleotide variants, represent an important yet underexplored dimension of microbial genetic diversity. These genetic alterations not only hold potential as differentiating biomarkers in samples but may also significantly impact microbial functions, including metabolic capabilities and interactions with the host. This database systematically analyzes Fusobacterium nucleatum-specific single nucleotide variants in CRC patients, laying a foundation for early diagnosis and targeted therapy.

The advancement of drug development and tumor immunotherapy has spurred the emergence of numerous promising anti-tumor vaccines. These biological agents achieve personalized, low-toxicity tumor immunotherapy by activating or enhancing the body's specific immune response to tumor antigens, representing a crucial breakthrough in overcoming traditional treatment limitations. However, the high heterogeneity of tumors, complex immunosuppressive microenvironments, and host variability continue to pose multiple challenges for the development, optimization, and clinical translation of anti-tumor vaccines. To conduct in-depth and systematic research on the mechanisms of action of anti-tumor vaccines, researchers have constructed the Anti-Tumor Vaccine Database, an integrated scientific resource. This database comprehensively catalogs antitumor vaccines approved for market release or undergoing clinical trials worldwide, covering diverse vaccine types including peptides, viral vectors, genetically engineered vaccines, and personalized vaccines to meet therapeutic and research needs across multiple tumor types. Simultaneously, the database multidimensionally integrates key information including antigen composition, mechanisms of action, immunogenicity characteristics, clinical indications, and vaccination strategies. Through systematic organization and standardized presentation, this resource assists researchers in vaccine mechanism analysis, immune response profiling, and clinical efficacy evaluation. It further supports vaccine optimization design, combination therapy strategy development, and predictive biomarker discovery, propelling tumor immunotherapy toward precision and safety.

Biological response modifiers (BRMs) are a new type of anti-tumor drugs. Clinically, they are classified into five major categories: cytokines, bacterial preparations, tumor proliferation viruses, thymosin, and traditional Chinese medicine preparations. BRMs exert their biological activity through four pathways: activating the activity of immune effector cells such as T cells, reducing the levels of inhibitory factors such as transforming growth factor, enhancing the expression of surface antigens on tumor cells to improve immune recognition ability, and inducing abnormal cells to differentiate normally. BRMs can achieve the following functions: enhancing the body's anti-tumor ability, inducing tumor cells to differentiate and mature into normal cells; reducing immune suppression effects, enhancing the body's tolerance to toxic substances, and directly enhancing the body's defense ability; enhancing the efficacy of chemotherapy, radiotherapy, and surgical treatment on tumors and reducing their side effects. Currently, BRM therapy is still in its infancy and is often combined with traditional radiotherapy in clinical practice, which can significantly increase the five-year survival rate of patients. It offers us more methods and possibilities for treating cancer, and we hope that in the near future, people will no longer be terrified of cancer.